Blog Archives
Numbers Lie

We don’t always realize it, but each one of us had come a long way since diabetes first came into our life. It doesn’t matter if it’s been 5 weeks, 5 years or 50 years, you’ve done something outstanding diabetes-wise. So today let’s share the greatest accomplishment you’ve made in terms of dealing with your diabetes. No accomplishment is too big or too small – think about self-acceptance, something you’ve mastered (pump / exercise / diet / etc.), making a tough care decision (finding a new endo or support group / choosing to use or not use a technology / etc.). (Thanks to Hilary of Rainie and Me for this topic suggestion.)
One thing I can say 100% for sure is that diabetes has made me better at math. Addition, subtraction, multiplication, division, graphs, patterns, fractions, confidence intervals… those things that I hated in school came back to rule my life.
You’ve heard the saying “numbers don’t lie” before, I’m sure of it. One of my most recent victories has been understanding that number can, in fact, lie. Most medical professionals want to know one number for people with diabetes: the A1c. Here’s my A1c history since my diagnosis less than two years ago:
- August 2011: 11.3 at diagnosis
- September 2011: 8.3 (big drop!)
- February 2012: 5.9
- August 2012: 6.1
- March 2013: 6.2
I parroted these numbers to medical professionals when asked and was judged on them. In fact when the 8.3 was reported, I got scolded by a PCP (who I won’t be seeing again) for such a “high” A1c. She saw that 8.3 in a vacuum. She didn’t see the diagnosis date one month prior and she didn’t see the massive 3-point drop. Likewise, I was praise by other members of my medical team for the 5.9… but what they didn’t know about those two numbers were that they were lies. LIES!!
The 5.9 reflected a lot of changes in my basal rates, my carbohydrate ratios and diet. It reflected a lot of low blood sugars. It didn’t reflect excellent numbers all the time. It wasn’t a real representation of my diabetes management. What the last two number reflect are a better grasp on my numbers, new insulin and the introduction of a CGM. They’re stable. Admittedly, they’re pretty good. Even if it’s not my personal goal.
Numbers other than A1c values can lie also. For example, this morning I had a reading of 77 but I felt like I was 27. Since meters are only required to be accurate within 20%, I could have actually been in the low 60s. Prices for our supplies can even lie, if you look at an insurance EOB you can see that.
Honestly, accepting the fact that numbers can lie is only a tiny accomplishment in my life with diabetes, but I was thinking about it today. Bigger D-accomplishments include:
- Advocating for my own health when I need to
- Educating others when I have the opportunity
- Getting every high blood sugar back into range and appropriately correcting the lows
- Giving myself that first shot
- Pushing the paperwork through to get on my OmniPod and Dexcom
- Having a normal life with a chronic health condition
- Making it on time to doctors appointments without the aid of a personal assistant
To read other accomplishment posts, go here.
Related Posts:
A memorable day
I’ve said several times before that I really don’t know people in my “real life” with type 1. I finally had the opportunity to meet DOC member Amy in person and discovered how truly small the world is (we found out that she’s known members of my family longer than she’s “known” me!). When I read today’s prompt directly followed by some tweets about diabetes in the wild, I thought back to a day… not my most memorable day with diabetes but one worth sharing.
Today we’re going to share our most memorable diabetes day. You can take this anywhere…. your or your loved one’s diagnosis, a bad low, a bad high, a big success, any day that you’d like to share. (Thanks to Jasmine of Silver-Lined for this topic suggestion.)
I was diagnosed with diabetes in the middle of August 2011. My husband and I moved to Cleveland in September and that October we were shopping at Crocker Park (an amazing outdoor shopping center). I wasn’t yet on an insulin pump but was in the process of getting started with one.
Brad and I had finished our shopping and were returning to our car in the parking garage. When we reached our garage, there was a group of three teenagers talking and laughing in the stairwell. The girl who was sitting on the step scooted over so we could walk past, as she scooted I saw it. It looked like a purple pager clipped to the outside of her pocket with a clear tube sticking out of it.
I wanted to exclaim, “I have diabetes too!” but the calm, rational adult in me reminded me that having a stranger point out your medical condition as a teenager could possibly mortifying, so instead I smiled and said thanks to her when we passed.
On the second level of the parking garage, when we were safely out of earshot I turned to Brad and said, “That girl on the steps has diabetes too and she was wearing an insulin pump.” He hadn’t noticed.
I learned two things that day:
1. There were other people in the world having “normal” lives while having diabetes. I hadn’t yet achieved a “normal” life since my diagnosis.
2. It’s completely possible to for the condition that had taken over my life to go completely unnoticed by others.
Sometimes I wish I had said something to the girl in the stairwell, especially after moments when my insulin pump being visible helped others feel less alone.
Other Memorable Days:
D-Blog Week: Share and Don’t Share
Last year, I double-timed it for D-Blog Week. This year, I’ll see what I can do.
Often our health care team only sees us for about 15 minutes several times a year, and they might not have a sense of what our lives are really like. Today, let’s pretend our medical team is reading our blogs. What do you wish they could see about your and/or your loved one’s daily life with diabetes? On the other hand, what do you hope they don’t see? (Thanks to Melissa Lee of Sweetly Voiced for this topic suggestion.)
When I go to any of my doctors, I feel like I turn into “super patient” and answer all questions precisely as if I’m being tested and just let the medicals lead the appointment. I’m married to a man with “white coat syndrome” so I know that’s not my issue, my issue is that I need to take control of my appointments. I did better at my last endocrinologist appointment, when I started a sentence with “while we’re talking, I need to ask you about travelling.”
I try to schedule my appointments online so it’s handy that I can type into the comments/reason for appointment box what I need to talk about and it ends up on my chart… whether or not that gets seen before I do, I don’t know.
Look at that! I’ve already strayed from the prompt!
What I wish they could see.
I wish they could see the life around my numbers. I mentioned about a year ago that I had an issue with a resident fixating on a string of low numbers and kept trying to change my basal programs to avoid them and somehow she didn’t understand they were outliers (because three days with lows in a row couldn’t be an outlier when you’re painting an entire house!). I explained over, and over, and over that those were not normal numbers. At that very point in time I wished I could snap her back to those days movie style so she could watch not only how active I was, how on top of treating those lows I was.
I wish that my healthcare team could see the things that I may not think to tell them about. I’m “new” at this whole living with diabetes thing and don’t always identify things they should know about. Although I doubt they should know about my sore neck from sleeping oddly, but I bet they should know about the tingly feeling in my hands that I only get in the mornings.
What I don’t want them to see. Read the rest of this entry
Diabetes Hero
Diabetes Blog Week Post #7
As the week of prompts comes to a close, we’re supposed recognize someone important in the realm of diabetes.
I could take this post and talk about the doctor who diagnosed me or the CDE who has answered endless questions, the phlebotomy who put up with my fear of needles or countless other medical professionals who’ve been a part of my diabetes management.
But…
I think this is an excellent time to talk about the night I came home from the hospital.
After the hours of waiting, frustration and uncertainty about going home, my sweet nurse came in and removed my IVs and told me to go ahead and get dressed (real clothes?! Amazing!) because I was going to get to go home before her shift ended. She left to get my discharge order signed and prescriptions written. My husband returned from his dinner in the cafeteria to find me dressed and waiting in my chair. With follow-ups scheduled and prescriptions in hand, I gulped down the last gross cup of potassium, signed a bunch of paperwork and was wheeled out of my room to the elevator.
When we arrived home, Brad got me fresh clothes and a towel and sent me off to take the best shower of my life.
My in-laws were waiting in the living room when I was finished. We were in dire need of groceries since I’d been so sick for so long and Brad was living at the hospital and merely sleeping at home. Arrangements were made for my mother-in-law to accompany Brad to the pharmacy and grocery store and my father-in-law and brother-in-law would stay with me until they returned.
While Brad and his mom were out, life felt a tiny bit like normal. Those of us back at the ranch watched the movie Despicable Me. When they had returned with groceries and insulin, we reviewed the food against my dietary orders then put it all away and figured out my life for the next few days.
Then came the moment of truth. Read the rest of this entry
It kind of looks like…
Diabetes Blog Week Post #6
Today’s topic: Snapshot Saturday
I’m not typically a weekend blogger, but I couldn’t skip this weekend (or last weekend for that matter).
The point of today is to share with you what diabetes looks like on a daily basis. So what does daily diabetes management look like?
It kind of looks like math:
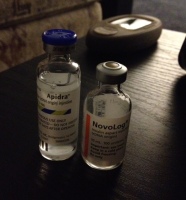
It kind of looks like a medical show: Read the rest of this entry
What They Should Know
Diabetes Blog Week Post #5
Today’s Topic: What they should know
I get to do what I usually do when I blog about diabetes, I get to say what I think everyone should know about diabetes.
I want people to know everything about diabetes. Actually I want to know everything about diabetes, but there’s too much information all around to cram into people’s brains during the maybe two minutes of their attention I have.
There are too many things to pick from, but I think I’ll select the umbrella… a definition.
Type 1 diabetes is a chronic medical condition, caused by an autoimmune reaction that attacked the insulin-producing cells in my pancreas and I will live with it for the rest of my life.
(Also see: My immune system ate my pancreas)
I’ve been asked a lot of questions after telling people about what type 1 diabetes is. Including:
- Can’t they just take out your pancreas?
- Will you always be on insulin?
- Aren’t you too young/old/skinny to have that?
- Can you still eat ____?
But when I really think about, it’s more and more apparent that I just wish people would come at diabetes with an open mind. Forget the things they think they heard one time and listen to someone who lives it.
I’ve encountered people who have tried to teach me about my own medical condition because they once knew someone who had diabetes. We live with this condition day in and day out. We work with medical professionals to decide our care. We are in charge of our own day-to-day treatment.
Diabetes blog week
Post #1: Find a Friend
Post #2: One Great Thing
Post #3: One Thing to Improve
Post #4: Fantasy Diabetes Device
Fantasy Diabetes Decive
Diabetes Blog Week Post #4
Today’s Topic: Fantasy diabetes device
Oh boy there are so many things I want (aside from a fully functioning pancreas, duh).
It’s no secret that I’ve been trialing a Dexcom (continuous glucose monitoring system). I kind of like it, the arrows tell me where I’m going and it alerts me to danger, but it’s another cell phone sized device, it’s another plastic piece and adhesive pad stuck to me. I know I’m not alone in wanting a closed loop system.
I kind of wish it would all be integrated with an app like our universal remote system is at home. (I mean seriously, I can use one iPad/iPhone/Android app to control the TV, DVD player, other DVD player, Apple TV and probably even my neighbor’s stereo.) If they can make a glucose meter that plugs into my iPhone, can’t they just make that work with my OmniPod and receive Dexcom readings and automatically talk to each other?
While we’re talking about apps, Read the rest of this entry
One thing to improve
Diabetes Blog Week Post #3
Today’s Topic: One thing to improve
I patted myself on the back for being responsible yesterday but now I get to confess what I need to do better (we all have room for improvement in our lives).
I can improve my Attitude
I have an attitude problem. This weekend I got incredibly frustrated because diabetes decided to kick me, repeatedly, to remind me that it’s still there. I had been riding wave of glorious blood sugars for days and was feeling pretty confident with my rates and my trial Dexcom was confirming that.
Until it wasn’t.
My blood sugar climbed into the 200s, I corrected. It still climbed. Corrected again. Still climbing. I rage bolused again and it finally came into a normal range just in time for dinner. Rinse and repeat.
I thought after a day of highs, I had gotten it down before bed and I’d wake up to a new day.
It was a new day during which, even looking at food caused a steady rise.
It’s exhausting, disheartening and infuriating. It’s defeating. I feel defeated when my numbers run out of control, paying no attention to the flood of insulin in my system. I adopt an attitude of failure. I’d like to quite diabetes. Or shake it senseless. But I can do neither.
I can change my attitude.
But it takes time.
Diabetes Blog Week
Post #1: Find a Friend
Post #2: One Great Thing
One Great Thing
Diabetes Blog Week Post #2
Today’s topic: One Great Thing. I’m supposed to give myself credit for doing something well with my diabetes management.
I’ve mentioned that I’m a perfectionist before. I feel like that helps me keep on top of things overall.
- I never leave home without my diabetes bag
- I test regularly
- I count carbs or guess as accurately as possible
- I keep my work emergency kit stocked
- I never let myself run out of supplies
I may try hard to be perfect, but I sometimes fail. The one thing that I’m great at though is driving with diabetes. By that I mean that I will not leave the house if I’m low or going that direction. I’ve been known to work late because I can’t get behind the wheel until my blood sugar comes back up.
Driving while low is incredibly dangerous and it hurts every time I see a news story about a erratic driver and they release that the driver was having a “diabetic reaction” or “diabetic emergency” because there’s always some idiot commenting that people with diabetes shouldn’t be allowed to drive or that they know that person wasn’t taking care of him or herself because a “good diabetic” wouldn’t have that problem. It spread ignorance and I have absolutely no desire to be that news story. (I probably have more to say on that topic, but we’ll save it for another day.)
Testing before driving can’t prevent your blood sugar from dropping while you’re behind the wheel, that sometimes means pulling over to do another finger stick. That is one reason I like the CGM that I’m trialing, I can check it at stop lights and see if my numbers are climbing, falling or holding steady.
Give Yourself Some Credit
I really like this topic because sometimes we have to remember that there are things we do well. Giving yourself credit where credit is due is important with any chronic medial condition.
Diabetes Blog Week
Post #1: Find a Friend









Petitions: We Shouldn’t Need Them
May 14
Posted by Probably Rachel
Today’s D-Blog Week topic is about petitions. Here’s the prompt:
Recently various petitions have been circulating the Diabetes Online Community, so today let’s pretend to write our own. Tell us who you would write the petition to – a person, an organization, even an object (animate or inanimate) – get creative!! What are you trying to change and what have you experienced that makes you want this change? (Thanks to Briley of inDpendence for this topic suggestion.)
This prompt inspired thoughts not related to writing a petition but about the fact that we shouldn’t need them. Not that long ago, a petition to standardize TSA screenings for people with self-monitoring medical equipment failed to reach the required number of signatures to move forward. This disappointed me. I wrote about my experiences flying out of Cleveland with TSA and the multiple refusals to be scanned, and the not terrible pat down. My security experience flying out of Seattle was in some ways worse and some ways better. Had the petition been successful in its goals, the overall flying experiences of people with diabetes would be better, but we shouldn’t have needed a petition in the first place.
The travel story:
Are you ready to be scared? I again turned down the body scanner at the airport and respectfully requested a pat down. I again received the “it’s totally safe lecture” this time a little more sternly. I was then sent through the metal detector, didn’t set it off and TSA agent number two was about to just let me go about my business when Agent #1 yelled, “she’s wearing an insulin pump!” Read the rest of this entry →
Posted in Commentary, Community
5 Comments
Tags: Advocacy, DBlog Week, Dexcom, Diabetes, education, OmniPod, petitions, Type 1 Diabetes